What Are Biological Indicators
Biological indicators , as defined by ANSI/AAMI and ISO, are test systems containing viable microorganisms providing a defined resistance to a specific sterilization process. A biological indicator provides information on whether necessary conditions were met to kill a specified number of microorganisms for a given sterilization process, providing a level of confidence in the process. Endospores, or bacterial spores, are the microorganisms primarily used in BIs. They are considered some of the toughest ones to kill. Additionally, bacterial spores are chosen for a specific sterilization process based on their known resistance to that process. For example, Geobacillus stearothermophilus spores demonstrate a high resistance towards steam and vaporized hydrogen peroxide and are therefore used in BIs that monitor these sterilization processes.
Monitoring Steam Sterilization Cycles Using Biological Indicators
Generally a biological indicator for evaluating moist heat sterilization will contain viable spores of Bacillus subtilis, Bacillus atrophaeus or Geobacillus stearothermophilus.
BI growth evaluation determines the viability of Bacillus spores after exposure to the sterilization process. This method is performed by placing spore strips or inoculated process control devices into sterile broth or in the case of BIs contained with their own medium system, the medium is released to contact the BI. All results are compared against an untreated spore strip or BI control.
For routine use, it is normal to examine for presence or absence of growth to ensure the sterilization process was performed adequately. It is important to include a positive control with the group of process indicator BI.
References
Sample Requirements
Viable BI sent for verification counting are recommended to be sent in triplicate. BI and PCD should be sent in contained vessels.
Glass vials should be wrapped to prevent cracking. Untreated BI to be sent and tested in conjunction with sample as a control
Fastening Bis Pitfalls And Tips
There are many ways to fasten BIs to your thermocouples, depending upon your specific activity. For example, utilization of BIs can vary from creating new loads for an autoclave or for a steam-in-place for a Bioreactor and transfer lines. It also depends on what type of materials are available . The main idea here is to secure the BI while still allowing steam penetration. In an autoclave you have virtually no chance to overly damage/lose BIs because they are usually in tubing, autoclave bags, assemblies, etc. versus a steaming process in a transfer line. In which case, the steam and condensate flow in the lines can damage your wet BIs and also potentially damage your BI fastener causing you to lose them in the lines. For example, fastening a BI with the improper tie wraps could melt the tie wraps to the BIs and piping.
Don’t Miss: What Does The Word Of Mean In Math
Types Of Biological Indicators For Sterilization Processes
There are various types of biological indicators depending on the need and sterilization process. The most common type is self-contained biological indicators . These indicators combine the carrier material with spore and growth medium into a single vial, eliminating the need for aseptic transfer.1 Following sterilization, the vial is activated allowing the spores to mix with the growth medium and incubated to allow spore growth. Some SCBI designs use an enzyme-based detection system that can detect enzyme activity faster, with shorter incubation times.
Irrespective of the design, biological indicators are used during a steam sterilization process, hydrogen peroxide sterilization process or ethylene oxide process, to ensure the efficacy and lethality of the process.
So Then What Is A Chemical Indicator
Chemical Indicators are used to be certain that packs are getting completely covered, and properly penetrated with steam. There are regular chemical indicators, and there is chemical indicator tape. The CI Tape is placed on the outside of the pack to indicate that the packs have been properly covered with the steam during a cycle. And the Chemical Indicator goes inside the pack to ensure proper penetration so you know the instruments have been hit and sterilized with the steam.
Tuttnauer actually offers 20-minute biological indicators, as well as 1-hour biological indicators. These are the only indicators you need to test gravity, pre and post-vac units.
Recommended Reading: Multiple View Geometry In Computer Vision
Evaluation Of Biological Indicators And Sterilization Process
A biological indicator is defined as a characterized preparation of a specific microorganism that provides a defined and stable resistance to a specific sterilization process. Biological indicators can be used to:
- assist in the performance evaluation of the sterilization equipment such as the autoclave
- monitor established sterilization cycles and in periodic re-validation of sterilization process.
Integrated Chemical Indicator Strips
Integrated chemical indicator strips provide a limited validation of temperature and time by displaying a color change after exposure to normal autoclave operating temperatures of 121ºC for several minutes. Chemical color change indicators can be placed within the waste load. If the chemical indicators fail on two consecutive loads, notify your Department Safety Manager.
Also Check: Are Men Biologically Stronger Than Women
Role Of Chemical And Biological Indicators In Infection Prevention
Proper sterilization monitoring requires a combination approach using mechanical, chemical and biological indicators.
This course was published in the September 2021 issue and expires September 2024. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
After reading this course, the participant should be able to:
While oral health professionals acquire baseline knowledge and meet clinical competencies related to infection prevention during their formal education, continuing education is critical to providing safe care. In todays practice setting, safe dental visits encompass new COVID-19 protocols, as well as existing infection prevention measures including verification of sterile instruments. While the U.S. Centers for Disease Control and Prevention recommends verifying dental instrument sterility, the Occupational Safety and Health Administration formally requires it. Proper sterilization monitoring includes using a combination of mechanical monitoring, chemical indicators and biological indicators .1,2 This paper focuses on sterilization processes, including the effective use of CIs and BIs.
What Is A Process Challenge Device
A process challenge device has historically been in a form of a BI placed into a package such as a test pack consisting of a biological indicator placed in a Tyvek® pouch. A PCD provides a challenge greater than or equal to your most challenging instrument to sterilize. At ASP, weve provided a single PCD which combined the most-difficult-to-reprocess devices and the worst-case conditions for each cycle to assure sterility.
In development of each STERRAD® sterilization cycle, simulation of the worst-case scenario included:
You May Like: What Does Biological Age Mean
What Is A Biological Indicator
A biological indicator is a preparation of one or more spore-forming microorganisms that have resistance to being killed during sterilization. The spore-forming microorganisms used in biological indicators are well characterized and selected based on the sterilization process being tested. Spore-forming microorganisms are used as BIs because they are exponentially more difficult to kill during sterilization than non-spore-forming microbes or spore-forming microbes in an active state. Furthermore, spore-forming microbes represent a minimal subset of the actual bioburden on items to be sterilized. Thus, if a sterilization process can destroy the bioburden of a product represented entirely as spores, the sterilization process will be able to kill all microbes in a worst-case bioburden situation. The biological indicators ability to mimic worst-case bioburden scenarios is how BIs validate sterilization processes and prove that a process is effective enough to sterilize a product in its final package consistently. Other common sterilization processes validated with BIs are the sterilization of manufacturing equipment and packaging components. BIs are also used to monitor and reassess sterilization processes for their effectiveness periodically.
Standards For Chemical Indicators
The International Organization for Standardization issues many standards for sterilization processes. Chemical indicators must adhere to these manufacturing and application standards, and guidance documents.
- BS EN ISO 11140-1:2009
- ANSI/AAMI ST60:1996
The most current standard is ISO 11140-1:2014. It defines 6 different types of chemical indicators for sterilization.
Read Also: What Is Corrosion In Chemistry
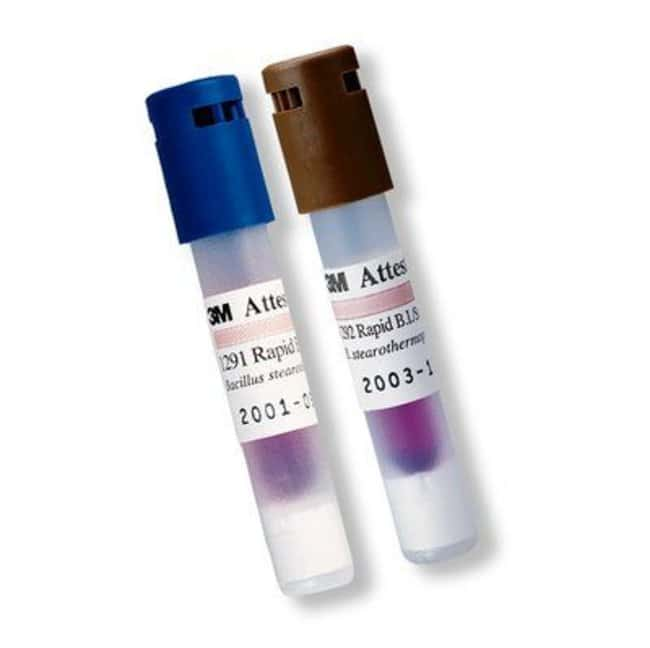
Biological Indicators For Steam Sterilization
Biological indicators are often used for routine monitoring, qualification and load monitoring of a steam sterilizer. Biological indicators are designed to demonstrate whether the conditions during a steam cycle were adequate to achieve a defined level of microbial inactivation. For steam sterilization, BIs are typically used within PCDs and AAMI ST79:2017 recommends using PCDs weekly, preferably daily, for monitoring sterilizers and in every load containing implants.
The PCD containing the BI and/or a chemical indicator should be placed in the most challenging location in the chamber. In a steam sterilizer, this is typically on the bottom shelf near the drain. Upon completion of the cycle, the PCD is taken out and the BI is incubated. After incubation the BI result is read. Incubators or readers will provide a final pass or fail result within a specified amount of time.
As per AAMI ST79:20172, PCDs containing biological indicators should be used for routine monitoring of steam sterilization cycles at least weekly, preferably daily, and in every load containing implants. Sterile Processing Department staff should follow the manufacturer’s directions for the appropriate placement of the PCD containing the BI in the sterilizer.
Besides routine sterilizer monitoring, PCDs containing BIs are also used for other applications as listed below:
Evaluation Of Biological Indicators
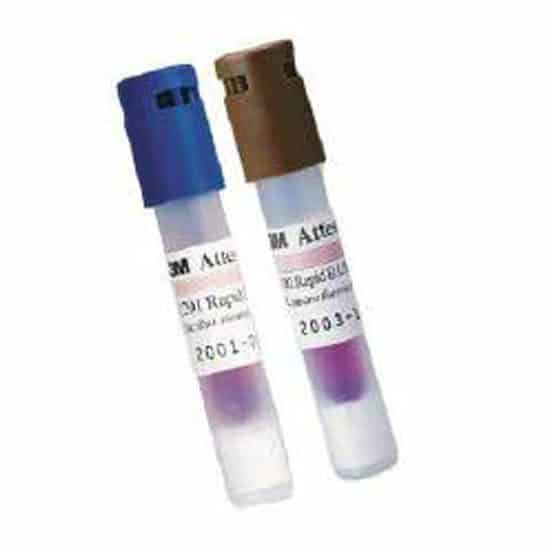
Each new batch of biological indicators that are used in good manufacturing practices operations should be qualified by performing a population verification count. A count ensures the count recovered meets manufacturers claims of the Bacillus population inoculated on the carrier. Counts are performed by resuscitation of the Bacillus, serial dilution and pour plate method.
Biological indicators evaluation and count tests are conducted in accordance with manufacturers instructions or USP < 55> Biological Indicators Resistance Performance.
Don’t Miss: What Is Arousal In Psychology
Where To Buy Biological Indicators
Healthcare facilities should purchase BIs from a reliable, accessible source for easy reordering. Biological indicators can be purchased from companies that offer sterilization and infection prevention products. Factors that may be considered when deciding which biological indicators to purchase include incubation time, brand name, cost, range and variety of products, validated applications and ease of use. Refer to ISO 11138-7:2019 for more information on supplier selection.
12 ANSI/AAMI ST79:2017 Comprehensive guide to steam sterilization and sterility assurance in health care facilities. Association for the Advancement of Medical Instrumentation 2017
Regulatory Guidance For Sterilization
As noted, effective sterilization monitoring requires a multifaceted approach using mechanical monitoring, as well as CIs and BIs. Several infection control recommendations related to CIs and BIs are outlined in the comprehensive 2003 CDC guidelines, which remain the gold standard in dentistry.1 The CDC guidance is broad and allows for flexibility in the implementation of its recommendations. Dental practices implement these recommendations in myriad ways, as CDC does not provide specific instructions as to how to carry out infection controls tasks. However, this flexibility results in little standardization in dentistry as compared to medicine. There is very little oversight unless infection control breaches are reported.
Ensuring that sterilizers are functioning properly is critical for safe practice and eliminating the spread of disease. External accrediting bodies in healthcare use AAMI ST79 to ensure standardization of sterilization procedures, as it provides a means for external oversight and reporting. Although AAMI ST79 is not required in dentistry, it is an excellent supplement to OSHA and CDC guidance.
Don’t Miss: Lesson 9.5 Geometry Answers
How Does A Biological Indicator Work
Actually, with the system now available from Tuttnauer USA, it is quite simple. Just take the biological indicator and place it in the lower right-hand corner of the autoclave you are testing. That is the most difficult spot for an autoclave to sterilize properly. Next, you run a complete cycle as you normally would. If the biological indicator passes with a positive from that position then you know all the bacteria in your instruments have been eliminated.
Iso Types Of Chemical Indicators For Steam Sterilization
ISO 11140-1:2014 classifies chemical indicators for autoclaves and sterilizers as follows:
- Type 1: Process Indicators
- Type 5: Integrating Indicators
- Type 6: Emulating Indicators
The types are not ranked by level of importance. Type 1 is not better than type 6. Each type simply denotes performance characteristics and intended use of chemical indicators.
ISO 11140-1:2014 section 4.1 “The classification structure used is solely to denote the characteristics and intended use of each type of indicator when used as defined by the manufacturer. This classification has no hierarchical significance.”
Since performance requirements are distinct, chemical indicators should only comply with one type. This chart summarizes the different ISO types of chemical indicators. It also provides examples of applications and STERIS Life Sciences products available for each type. Use it to help choose the correct chemical indicator for monitoring specific sterilization processes.
Recommended Reading: What Is Vapor Pressure Lowering In Chemistry
I Have Multiple Sized Practices Will One System Be Enough For The Larger One
Tuttnauer actually makes multiple sizes for different applications. There is a smaller incubator called the MiniBio designed for a physicians office or dental practices. And there is also a larger one called the BioNova for use in ambulatory surgical centers, hospitals, and larger facilities.
These incubators are programmable as far as times and documentation purposes. This is an extremely important function for AAMI guidelines. And they will also print if the biological indicator passes or fails. Tuttnauer is the only company that manufactures a unit that includes all those functions together. Others dont even offer the printout for keeping proper documentation.
The incubators are also able to do ST8 Challenge Packs for ambulatory surgical centers enabling them to more easily maintain their specific AAMI guidelines.
Which Biological Indicators Should Be Used For Each Sterilization Process
Biological indicator selection is based on the resistance of the BI to the sterilization process. The BI system must provide a greater challenge to the sterilization process than the native bioburden of the product being sterilized. The biological indicator suggestions by sterilization process below represent the most common choices. However, other biological indicators may be used with appropriate justification. Overall, the typical BIs are spore-forming bacteria of the genera Geobacillus, Bacillus, and Clostridium.
Moist Heat Sterilization by Direct Contact
Moist heat sterilization of most non-liquid products is known as steam sterilization by direct contact. Steam sterilization traditionally uses spores of G. stearothermophilus as a BI. G. stearothermophilus is a microorganism that likes heat that has a moist heat resistance substantially greater than that of most active microorganisms. Note that active microorganisms are organisms not in their spore form.
Moist Heat Sterilization of Aqueous Liquids
For moist heat sterilization, heat-resistant spore-forming microorganisms such as C. sporogenes, B. subtilis, or B. atrophaeus are chosen as biological indicators. These spore-forming microorganisms are also preferred for verifying the sterilization of aqueous solutions due to their lower thermal resistance.
Dry Heat Sterilization
Ionizing Radiation
Gas Sterilization
Chemical Sterilization
Vapor Phase Sterilization
You May Like: How To Find Force Physics
Benefits Of Biological Indicators In Sterilization Process
Biological indicators, depending on the specific type, can be used for various sterilization processes using steam, hydrogen peroxide gas, ethylene oxide and more.
Several factors such as operator experience, load preparation and sterilizer condition can impact the sterilization cycle. BIs provide a direct measure of the lethality of the process and so the use of BIs to routinely monitor sterilizers provides assurance in the efficacy of the sterilization process.
BIs are typically used within process challenge devices that are designed to represent the most challenging products routinely processed. A passing result for the BI within this defined challenge demonstrates that the sterilizer is effective in killing a large number of highly resistant bacterial spores, providing users with a level of assurance in their sterilization process.
What About My Mail In Indicators That I Use Now
Practices like to believe that the mail-in program is cheaper. Actually it can be much more expensive, and it is also very insufficient where AAMI sterilization guidelines are concerned.
Consider this Test for a bacteria on Monday and mail your test in. Your results will be returned in approximately 4 to 6 days.
Now what if you get back a failed result?
That means for 4 to 6 days you have insufficiently cleaned instruments multiple times and used them on all the patients since. Now you have to spend all that time to contact all those patients that trusted you. And you have also put the practice at risk by compromising the care of those patients.
Its not difficult to see that it is much safer and monetarily sound to use a system in-house that gives you results at the end of every cycle you test.
Also Check: What Is Pcr In Biology
What Is The Difference Between The Two
A biological indicator is used to ensure the chamber of your autoclave is getting completely saturated in the sterilization process. And the Chemical Indicators are used to be certain the steam is covering the entire load, and that the instruments are receiving the necessary amount of steam for proper sterilization.
What Types Of Biological Indicators Are There
Some BIs contain a single microorganism species, while others contain two species and concentrations of bacterial spores to compare different sterilization processes. There are three primary types of BI indicators.
#1: Spores on a carrier
In this preparation, spores are placed on a carrier . The disks or strips can be paper, glass, plastic, metal, or other materials. BIs using a carrier are often packaged to maintain the integrity and viability of the inoculated spores on the carrier. Following sterilization, neither the BI carrier nor the BI packaging should be damaged or degraded.
#2: Spore suspension
Biological indicators can also be an inoculate spore suspension placed on the product being sterilized or into representative units of the product to be sterilized. A surrogate article that is substantially similar to the product being sterilized can be used if it is not practical to inoculate the actual product. For spore suspensions used in liquid products, the population and D value of the BI spore is critical to determine to evaluate the efficiency of the sterilization process.
#3: Sealed system spores
You May Like: Do You Need Organic Chemistry For Pt School