Whats Different About Hela Cells
There are 3 major differences between normal cells and HeLa cells:
1- HeLa cells are cancerous. The difference between normal cells and HeLa cells is most visible when you look at the chromosomes . HeLa cells, like many tumours, have error-filled genomes, with one or more copies of many chromosomes: a normal cell contains 46 chromosomes whereas HeLa cells contain 76 to 80 total chromosomes, some of which are heavily mutated , per cell. This is due to the Human Papillomavirus , the cause of nearly all cervical cancers. HPV inserts its own DNA into host cells and the additional DNA results in the production of a p53-binding protein which inhibits it and prevents native p53 from repairing mutations and suppressing tumours, causing errors in the genome to accumulate as unchecked cellular divisions occur.
2- HeLa cells grow unusually fast, even considering their cancerous state. Indeed, HeLa cells grow easily and rapidly, doubling cellular count in only 24 hours, making them ideal for large scale testing. They grow so fast that they can contaminate and overtake other cell cultures. This is related to the fact that Henrietta Lacks had syphilis which results in an aggressive growth of cancer due to a weakened immune system. And in 2013, it was shown that the scrambled HPV genome inserted itself near the c-myc proto-oncogene in Henriettas genome , causing its constitutive expression and the rapid replication of HeLa cells in her body.
HeLa cells are still widely used in research:
Significant Research Advances Enabled By Hela Cells
In 1952, HeLa cells became the first human cell line that could grow and divide endlessly in a laboratory, leading scientists to label these cells immortal. The immortality of HeLa cells contributed to their adoption across the world as the human cell line of choice for biomedical research. Though additional cells lines have been developed over the years, HeLa cells continue to be widely used to advance biomedical research and medicine.
The enduring use of HeLa cells in biomedical research is represented below through a timeline of events and scientific publications that describe research using HeLa cells. The timeline aims to show the role that HeLa cells have played in some of the major advances in fields such as cancer biology, infectious disease, fundamental microbiology and many others. The hyperlinked text provided in each entry provides the underlying sources for the advances and allows the reader to take a deeper look into the actual science. The events that were selected were based on the number of times researchers cited, or gave credit, to the publication in which the events were described. Research involving HeLa cells has been described in more than 110,00 scientific publications. This staggering number makes it clear just how important these cells have been to research over the past six decades.
JUMP TO DECADE
Salmonella
How Do Hela Cells Work In Biomedical Research
Scientists were studying human cells long before they started using HeLa cells. However, they had a lot of trouble keeping individual cell lines alive. A cell line refers to all the generations of cells produced from a specific culture of cells. Working with a single cell line allowed researchers to verify their results and build on previous research. But when all the cells in a line died, they had to start over with a new one.
Lacks cells were different. They provided researchers with the first immortal human cell line ever grown in a laboratory. Researchers originally took HeLa cells from an aggressive cervical cancer tumour. These cells never stopped reproducing. When given a constant supply of nutrients, they produced a new generation of cells in less than 24 hours.
HeLa cells grew so rapidly and so well that research could now be done much faster than before. As soon as scientists recognized their potential, HeLa cells went into mass production. They were produced at the worlds first cell factory. From there, they were made available to labs around the world.
- the cancer drug tamoxifen
Read Also: What Does Dependent Variable Mean In Math
Hela Cells: Origin Of This Important Cell Line In Life Science Research
If you work in Biology, youve most certainly heard of HeLa cells, as they have been around for over 60 years and are some of the most extensively used cell lines in Biomedical research. But where did these cell lines come from?
Henrietta Lacks
In 1951, Henrietta Lacks came into John Hopkins Hospital in Baltimore, worried about a lump in her abdomen, where she was diagnosed and treated for cervical cancer . She eventually died of her cancer later that year, without knowing what her cells would help accomplish.
The surgeon treating Henriettas adenocarcinoma had been collecting cancerous tissue samples from patients for research lead by Dr. George Gey, Director of the Tissue Culture Laboratory at John Hopkins. His objective was to cure cancer by creating an immortalized cell line for research, in order to develop therapies and medicines.
For years, Dr. Gey and his wife Margaret had been trying to cultivate human cells in vitro. All their previous attempts at growing human cells in a laboratory lead to the death of the cell cultures within a few generations. That is, until Henriettas tumour sample: HeLa, named after the two first letters of Henrietta and Lacks.
Important Ways Henrietta Lacks Changed Medical Science
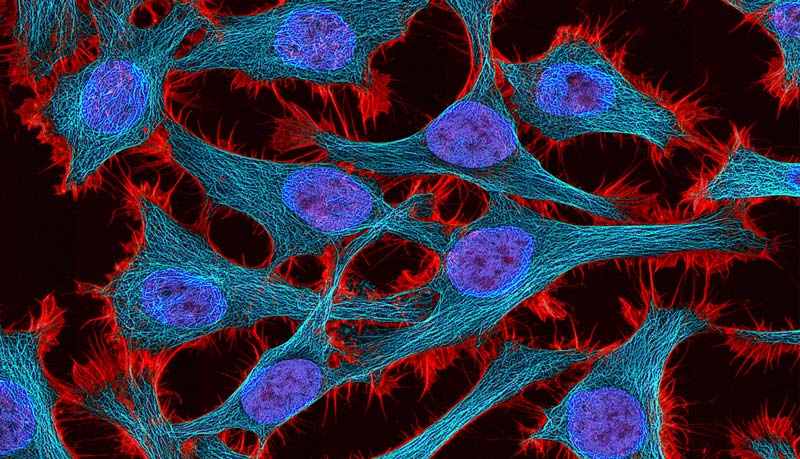
Henrietta Lackss cells have long been familiar to scientists but it was the ethical controversy around those cells that made her famous to the wider world.
Her fame was thanks to an award-winning book published in 2010 that explored how, in the course of Lackss treatment for cancer, doctors isolated what became the first immortal human cells. The HeLa cells survived, thrived, and multiplied outside her body, so much so that they have been in continual use in labs around the world for 65 years, even though Lacks herself succumbed to cancer in 1951. But their use has raised challenging issues about medical samples taken without consent and how individuals and their families should be compensated for discoveries based on their tissues.
Now, that story is the subject of an HBO movie coming out later this month, making it an opportune time to reflect on who Henrietta Lacks was and what her cells have contributed to science. Here are just a few of them.
Also Check: Hbo Child Of Rage
Hela Cells Contamination Issues And Significance
In 1967, works of Stanley Gartler, Ph.D. found that HeLa Cells had contaminated other human cell lines. This, as well as additional findings involving contamination, was an important discovery that influenced the reappraisal of tissue culture stocks by the ATCC and the Cell Culture Laboratory at the Naval Biosciences Laboratory.
The HeLa cell contamination had therefore brought to light an important culture contamination issue for the scientific community as a whole. For instance, according to one of the studies, cancer cell lines from human breast tissue were found to have intra and interspecies contamination.
From this and other studies, it became evident that a concerning percentage of all cell lines were not what they were deemed to be. Apart from issues of contamination, this discovery was also important in that it highlighted another important issue that of misattributing given property to a given cell line.
Through contamination of given cell lines by another, certain attributes of the contaminant could be misattributed to the cell line under investigation thus affecting the results of the study.
In scientific research, this was a real issue that had to be addressed. This discovery, therefore, was an important one in that it raised awareness and a need for better handling of biological samples to avoid contamination.
* HeLa cells have been referred to as laboratory weed in some spheres because of their persistent contamination of other cell lines.
Black History The Hela Cell And Cancer Research
Life is studied at the atomic and molecular scale in molecular biology, biochemistry, and molecular genetics. At the level of the cell, it is studied in cell biology. In biological and medical research, a HeLa cell is a cell that is derived from cervical cancer cells. A HeLa cell was taken from a Black woman named Henrietta Lacks.
This cell line was propagated for use in cancer research. Initially, the cell line was said to be named after a “Helen Lane,” in order to preserve Lacks’s anonymity. The cells proliferate abnormally rapidly, even compared to other cancers. HeLa cells have been transformed by the human papillomavirus 18 , and have different properties from normal cervical cells. They are used as model cancer cells and for studying cellular signal transudation. HeLa cells have proven difficult to control. They sometimes contaminate other cell cultures growing in the same laboratory, interfering with biological research.
On Oct. 4, 1951, Henrietta Lacks died of cervical cancer at Johns Hopkins University Hospital in Baltimore. But Lacks will live forever in laboratories and research centers worldwide that use her unique, immortal cells for medical research. The HeLa cells of her cancer, were the first human cells discovered to thrive and multiply outside the body, seemingly forever, allowing researchers to conduct experiments previously impossible.
Recommended Reading: Meaning Of Multiples In Math
What Is Henrietta Lacks Importance To Modern Medicine
HeLa, or Lackss cells, were the first immortal human cell line to be created using the first two letters of each of her names. The scientists at the hospital where she died, Johns Hopkins in Baltimore, had been trying for years to start a continuously reproducing cell line, but the cells never grew.
Hela Cells And Virus Research: Then And Now
HeLa cells were first used to study the growth and spread of poliomyelitis virus, the pathogen that causes polio. This research eventually led scientists to develop a vaccine for polio in the U.S. All children born in the U.S. now receive four doses of the inactivated poliovirus vaccine to prepare their immune system to fend off polio infections. Now, the worldwide incidence of wild polio has dropped 99% and is completely eradicated in the Americas, Europe, South East Asia, the Western Pacific, and, most recently, Africa. The Center for Disease Control projected that, in the absence of a vaccine, more than 17 million people would have been infected and paralyzed by the virus. Without HeLa cells, this projection may have become a globally morbid reality.
Figure 2: ACE2 receptors decorate the surface of HeLa cells to promote infection. HeLa cells do not naturally display high levels of ACE2 proteins on their surface, preventing efficient infection by SARS-CoV-2 particles. However, when researchers engineer HeLa cells to display the ACE2 protein, the viral particles gain entry into the cells and begin their cycle of infection.
You May Like: Is Physics Harder Than Math
Ways Henrietta Lacks Changed Medical Science
The controversial history of her “immortal” cells will be the subject of an HBO movie
Henrietta Lackss cells have long been familiar to scientists but it was the ethical controversy around those cells that made her famous to the wider world.
Her fame was thanks to an award-winning book published in 2010 that explored how, in the course of Lackss treatment for cancer, doctors isolated what became the first immortal human cells. The HeLa cells survived, thrived, and multiplied outside her body, so much so that they have been in continual use in labs around the world for 65 years, even though Lacks herself succumbed to cancer in 1951. But their use has raised challenging issues about medical samples taken without consent and how individuals and their families should be compensated for discoveries based on their tissues.
Now, that story is the subject of an HBO movie coming out later this month, making it an opportune time to reflect on who Henrietta Lacks was and what her cells have contributed to science. Here are just a few of them.
Creating The Field Of Virology
Over the years, scientists have infected hardy HeLa cells with various viruses HIV, herpes, Zika, measles, and mumps, to name a few to better understand how to battle them. They discovered, for instance, that the type of white blood cell called a T cell sports a surface protein called CD4, which is what HIV uses to enter the cell. When CD4 was added to HeLa cells they could be infected with HIV, allowing HIV drugs to be tested on HeLa cells.
Researchers also learned that the measles virus constantly mutates when it infects HeLa cells, making the disease harder to fight. More recently, microbiologists found that Zika cannot multiply in HeLa cells. Digging further into why that is could produce a new treatment or vaccine for the disease.
Also Check: Mcdougal Littell Geometry Worksheet Answers
How Are Hela Cells Being Produced
The HeLa cells multiply by mitosis. This is a life cycle that the cells go through, which causes them to divide and multiply. The cycle consists of several phases.
In the interphase, which itself is also divided into three phases, cell organelles, proteins and the cell grows. In addition, the genetic material is doubled and the cell is prepared for division.
In the M-phase the cell divides, new daughter cells are formed, which again enter the interphase. The cycle is repeated until the cells have differentiated.
A special section of the interphase is the G phase. The cells remain in this phase if they lose their division activity or if they do not pass the individual checkpoints of the interphase. This can happen, for example, if they are not the right size.
In order for the cells to multiply well, it is important that the cells are supplied with sufficient nutrients and have sufficient space to grow. Normally, cultivation is performed in a CO2 incubator at high humidity and a constant temperature of 37°C. It is very important to change the medium regularly, otherwise the cells will die.
Cultivation in large quantities is carried out by companies from which the HeLa cells can be ordered. Afterwards they can be further cultivated and multiplied for various experiments in our own laboratory as described.
Why Are Hela Cells So Special
Cancerous HeLa cells are found in the HeLa cells. The growth of HeLa cells is unusual, even considering their cancer-causing state. HeLa cells grow rapidly and easily, doubling their cellular count in only 24 hours, making them ideal for large-scale testing in the lab. The cells grow so quickly that they can contaminate and overtake other cells.
You May Like: Who Is The Biological Father Of Elton John’s Sons
What It Means To Be Immortal
Normally, human cell cultures die within a few days after a set number of cell divisions via a process called senescence. This presents a problem for researchers because experiments using normal cells cannot be repeated on identical cells , nor can the same cells be used for extended study. Cell biologist George Otto Gey took one cell from Henrietta Lack’s sample, allowed that cell to divide, and found the culture survived indefinitely if given nutrients and a suitable environment. The original cells continued to mutate. Now, there are many strains of HeLa, all derived from the same single cell.
Researchers believe the reason HeLa cells don’t suffer programmed death is because they maintain a version of the enzyme telomerase that prevents gradual shortening of the telomeres of chromosomes. Telomere shortening is implicated in aging and death.
Unsung Heroes In Science: Henrietta Lacks
While not a scientist, the first successful line of human cells grown in a lab came from a cancer sample from Henrietta, and have become instrumental in biological research.
Henriettas story has also prompted many ethical and moral questions about how scientific work is conducted
While Henrietta Lacks was not a scientist, the contribution that she has made to science has made a huge impact. The first successful line of human cells grown in a lab came from a cancer sample taken from Henrietta. These cells have been used millions of times in countless labs across the world and have had an invaluable contribution towards scientific discovery. Henriettas story has also prompted many ethical and moral questions about how scientific work is conducted, about the rights and uses of cells and tissue taken from patients and about the treatment of African-Americans and other marginalised communities in scientific and medical research.
Recommended Reading: Michael Jackson Biological Children
How Has Henrietta Affected And Changed Medicine
The collection of cells from Henrietta Lacks body by medical researchers after her death in 1951 changed the course of medicine forever. Her cells were collected by medical researchers after she died in 1951. These cells were named HeLa cells by the researchers. Medical research was changed by these cells.
Improved Cell Culture Practices
During the mass production and distribution of HeLa cells for polio vaccine testing at Tuskegee University, lead researchers Brown and Henderson pioneered new cell culture protocols, such as the use of rubber-lined screw-capped bottles and tubes and strict QC measures. The temperature sensitive nature of HeLa cells also led the researchers to use multiple incubators and introduce novel shipment solutions such as Equitherm and insulated shipping containers. After Gartlers discovery that HeLa cells could travel through the air and contaminate other cultures, vast improvements were made to cell culture practices, to prevent further costly cross-contaminations.
You May Like: Geometry Chapter 10 Test Form B Answers
Where To From Here
The story of Henrietta Lacks and HeLa cells generated tremendous public attentionparticularly around informed consent for biospecimen researchand has demonstrably influenced policy discussions in this arena. These have occurred in the context of rapid scientific and technological innovation and the inescapable recognition that complete deidentification of biospecimens and data is illusory. As a solution, proposed regulatory changes look prominently to routine consent for research use of biospecimens, regardless of whether they were originally collected for research or clinical purposes. These proposals are premised in part on public opinion data, although a closer look at such data reveals a complicated mosaic of perceptions and preferences. What lessons can we draw from all this about ethics and policy for biospecimen research?