Cumulus Cells And Follicular Fluid
Cumulus cells are implicated in oocyte development and competence . In addition to interacting directly with the oocyte to facilitate maturation, cumulus cells are also bathed within the same follicular environment during oocyte maturation, thus may retain a footprint to reflect its quality and potential to form a viable embryo . It has been proven that cumulous cells are useful for non-invasive diagnosis of oocyte quality . Next-generation sequencing on human cumulus cells has revealed that miRs represent the major small RNA type, constituting as much as 71% of the total small RNAs . As a way of interaction, it has been shown that bovine cumulus cells and oocytes reciprocally affect the abundance of miRs in each cellular compartment , and these miRs readily control gene expression with extensive downstream functional implications. Gene expression studies on human cumulus cells have revealed transcripts that may be involved in oocyte maturation, implantation, and pregnancy with their regulatory miRs just beginning to be realized . During IVF treatment, cumulus cells are retrieved while still firmly attached to each oocyte, and as such, their collection can be sourced from individual oocytes and, thus provide an indication of the developmental potential for individual oocytes.
Difference Between Fertilization And Implantation
The fusion of male and female gametes informs the zygote, whereas implantation is the method of blastocyst attaching to the uterus wall moreover, fertilization is a process that occurs after the implantation. It takes about 24 hours of evolution, whereas implantation occurs just after 8 to 10 days of fertilization.
Passage To The Uterine Wall
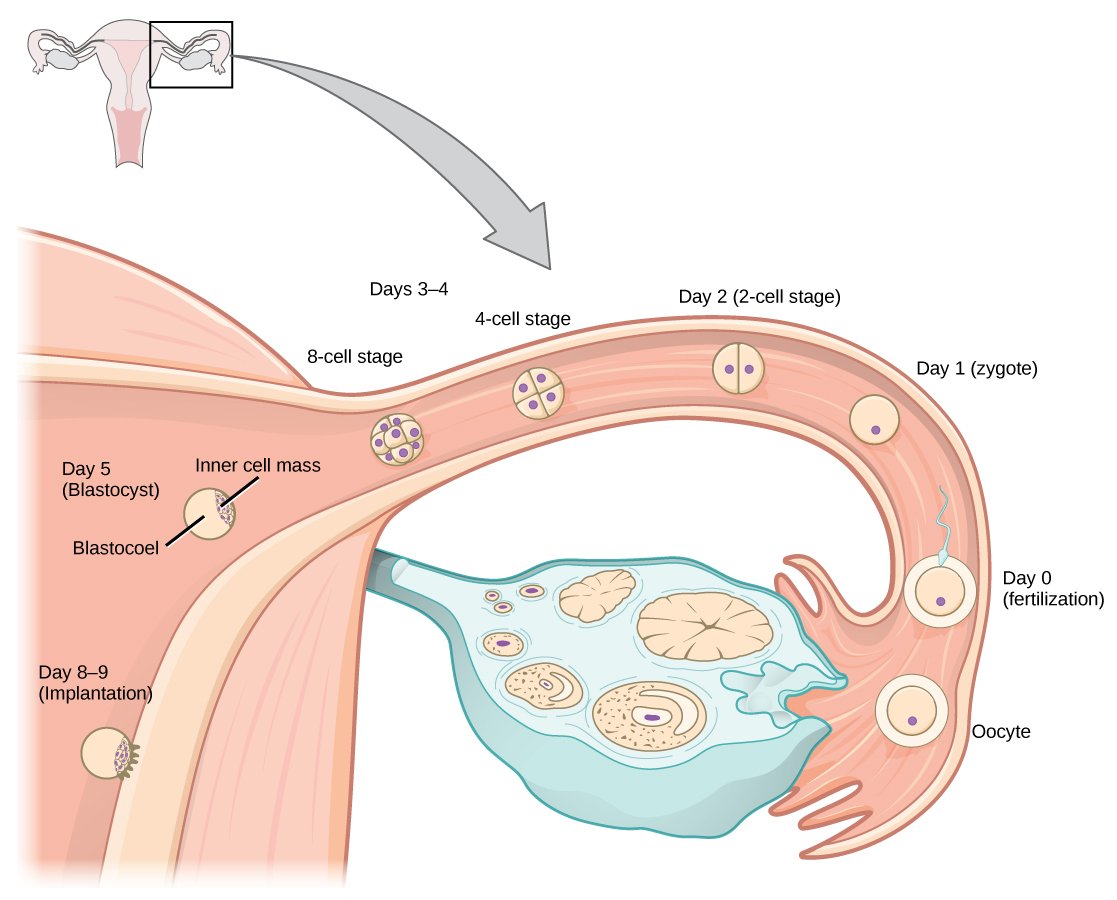
It takes about seven days for the blastocyst to find its way to the mammalian womb. Some drastic steps are taken in making this journey. Once a sperm enters an egg, a tough membrane called the zona pellucida forms around it that is impenetrable to other sperm. This is a protective mechanism against multiple sperms penetrating it. For reference, for any female egg there are between 40 million to 1.2 billion sperm cells competing for it in a single ejaculation. While this shield is helpful, it is not compatible with the growth of the new embryo. Therefore, the egg sheds off the zona pellucida between days five and seven as it begins to differentiate. This starts a rearrangement of cells on the outside and inside of the egg, and the eventual blastocyst forms.
This all takes place on the fifth day post-fertilization, after which the blastocyst travels down the fallopian tube. This is made possible with the help of cilia that contract, and move the egg into the uterus. Since the egg has to shed off the zona pellucida, it can now implant itself into the inner lining of the uterus called the endometrium. The microvilli on the surface of the trophoblast cells will adhere to the epithelial cells of the uterus through glycoproteins. Once they adhere, the fertilized egg and uterine lining can no longer be flushed out during the menstrual cycle.
Don’t Miss: Who Is Prince Jackson’s Biological Father
What Are The Symptoms Of Implantation
While undergoing fertility treatment, you constantly have a heightened understanding of your body. Subsequently, after the embryo transfer, you’ll be gaping for all feasible clues of big news regardless, the tokens of successful implantation can be relatively delicate.
As soon as the implantation occurs, some women will encounter some symptoms. These symptoms vary from woman to woman due to different ranges of hormonal imbalance in their body. Some common symptoms experienced by many women are listed as below:
Cramps – After the embryo implants, you will realize some distress. Each woman is distinct, and so not everyone realizes abdomen cramps. These are different than pre-menstrual cramps. Here the sensation is typically delicate and will barely linger a day or two.
Spotting – Implantation bleeding is given the name of Spotting. Several women face spots between 10 to 14 days after the conception. This is approximately the time around which you will expect your period.
Implantation is the indication that your fertility has occurred successfully, and you may come to be pregnant. Nevertheless, everyone is unique so there are limited more symptoms that some women may encounter. Here, we schedule some other symptoms of profitable implantation.
Sensitive Breasts: – After successful implantation, you might learn that breasts emerge swollen or sore. This occurs due to the changes in your hormone statuses.
1. What Happens During Implantation?
Laboratory Identification Of Mirs With Translational Potential For Implantation Prediction
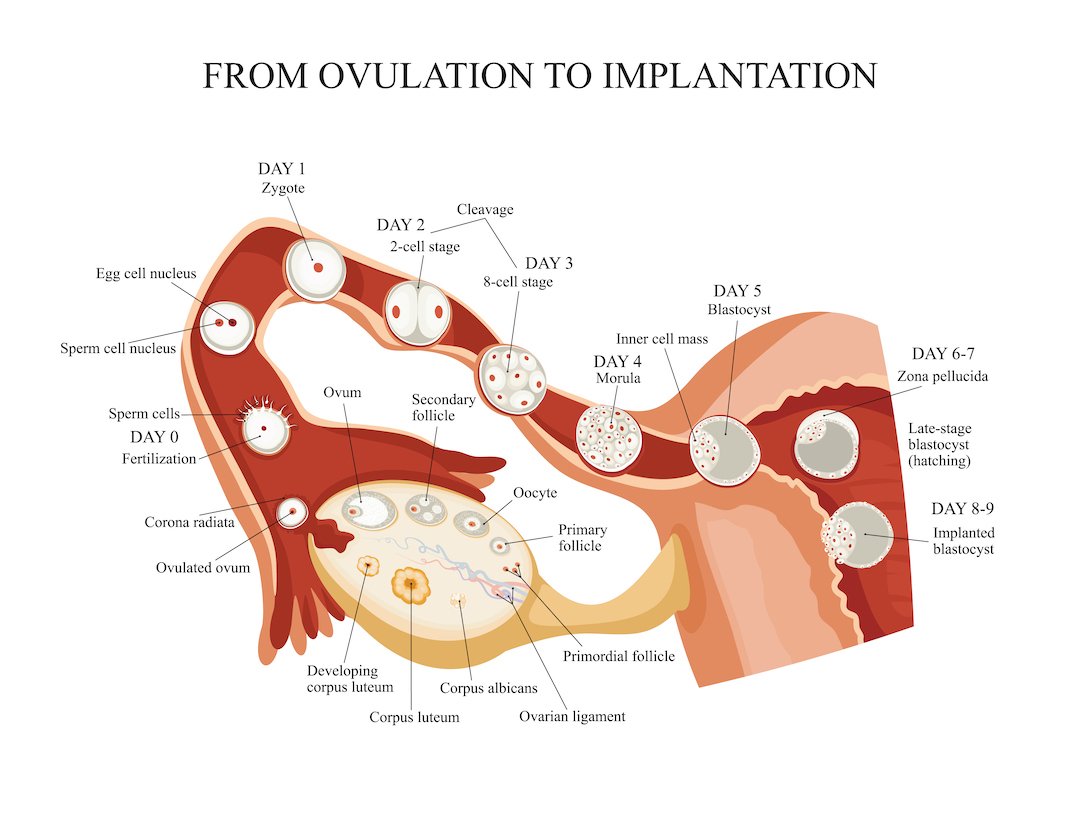
A standard IVF treatment broadly requires egg retrieval, sperm collection, IVF, and embryo culture before transfer. The collection of cumulus cells and follicular fluid is possible during egg retrieval without affecting IVF . Analysis of gene and miR expression in follicular fluid and cumulus cells indicates oocyte and embryo quality, thus the implantation potential from an embryos perspective . Embryos are generally cultured up to 56 days to reach the blastocyst stage before transfer . Embryos secrete specific profiles of miRs that may reflect their quality and implantation potential . The endometrial epithelium secretes factors into the uterine cavity to regulate implantation and uterine fluid, or uterine lavage washings can potentially be used to detect miRs as biomarkers for the prediction of receptivity and implantation . Blood contains extracellular miRs with expression levels of some miRs positively correlating with endometrial levels and can potentially indicate whether the endometrium is dysregulated or receptive . Abnormalities in sperm contribute to blastocyst development and quality , which could impact implantation. It has been shown in mice that sperm relays epigenetic information to the oocyte during fertilization and influences pre-implantation embryo and offspring development . The development of non-invasive biomarkers has driven extensive research in this area with an overall aim to improve the success rate of implantation and IVF treatment.
Also Check: Relationship In Math Definition
What Are The Different Types Of Fertilization
There are two different types of fertilization- internal fertilization, where the fusion of egg and sperm occurs inside the female reproductive tract, for eg., humans and external fertilization, where the fusion of male and female gametes occurs outside the body of the organism, for eg., sea urchins, frogs, etc.
What Is The Meaning Of Implantation
Implantation is established as the procedure by which the embryo ties to the endometrial surface of the uterus. It then invades the epithelium and the maternal circulation to build the placenta. In simple words, implantation can be defined as the early stage of pregnancy.
Before the onset of implantation, though both embryo and endometrium should embark a comprehensive process in a time- and location-specific path. Crosstalk between the receptive uterus and a competent blastocyst can altogether occur during a limited time interval, recognized as the window of implantation.
From the time of conception, your body undergoes a dramatic process of changes landing finally to the first pregnancy test. In all these, implantation is the most significant step. Implantation is regarded as an early sign of pregnancy.
After the egg is fertilized, it travels down the fallopian tube to the uterus. It divides into several multiples of cells that eventually grow into a cluster of 100 cells called a blastocyst.
Also Check: How To Find Ksp From Molarity
D Signaling By Growth Factors
The EGF-like growth factors interact with the receptor subtypes of the erbB gene family, which is comprised of four receptor tyrosine kinases: ErbB1 , ErbB2, ErbB3, and ErbB4. They share common structural features but differ in their ligand specificity and kinase activity . The initial dimerization between coexpressed receptors upon ligand binding constitutes the classical mechanism of action of EGF-like ligands. Spatiotemporal expression patterns of EGF gene family members and ErbBs in the uterus during the periimplantation period suggest compartmentalized functions of EGF-like growth factors in implantation .
Among many growth factors that have been studied in humans, HB-EGF appears to play a role in implantation and embryonic development. Its expression is maximal during the late secretory phase when the endometrium becomes receptive for implantation and cells expressing the transmembrane form of HB-EGF adhere to human blastocysts displaying cell surface ErbB4 . Furthermore, HB-EGF was shown to be one of the most potent growth factors for enhancing the development of human in vitro fertilization-derived embryos to blastocysts and subsequent zona hatching . Thus, cumulative evidence suggests that HB-EGF has a significant role in preimplantation embryo development and implantation as a paracrine and/or juxtacrine factor in various species.
F Homeobox Genes In Implantation
A recent study using microarray analysis further revealed that the absence of Hoxa-10 in the uterus in response to progesterone is associated with two cellular disturbances . First, among many genes that were up-regulated in the Hoxa-10-deficient uteri, two cell cycle molecules, p15 and p57, were notable. These two genes are both cyclin-dependent kinase inhibitors , suggesting that the previously observed defect in stromal cell proliferation in Hoxa-10 mutant mice could be associated with this up-regulation of CKIs. Second, the microarray experiments and follow-up fluorescence activated cell sorter analyses demonstrated that there was hyperproliferation of T lymphocytes in the Hoxa-10-deficient uterine stroma in response to progesterone. These results suggest that an aberrant lymphoproliferation has adverse effects on implantation in the Hoxa-10-deficient mice. In humans, both Hoxa-10 and Hoxa-11 genes are markedly up-regulated in the uterus during the midsecretory phase in steroid hormone-dependent manner , suggesting their roles in human implantation.
Don’t Miss: Kuta Software Infinite Algebra 2 Solving Inequalities Answers
C Discovery Of Novel Implantation
In humans, microarray technology has been used to examine uterine cell lines and explant cultures under conditions that simulate the periimplantation period . A more physiological application is based on estimates of the putative window of receptivity in women. Endometrial biopsies taken before and during this period have identified significant changes in a modest number of genes that may serve as markers for uterine receptivity in humans. Although some variation exists in their methods, two independent studies used the same microarray platforms for their analysis . A comparison of the results shows differential regulation of a small number of genes around the time of uterine receptivity for implantation . Interestingly, there are a number of these genes that are also differentially expressed in mouse models of implantation and uterine receptivity.
I Matrix Remodeling And Angiogenesis During Implantation And Decidualization
Tissue remodeling and angiogenesis are two hallmark events during implantation and decidualization. The changing endocrine state of the female during the reproductive cycle and pregnancy results in extensive remodeling in the uterine tissue . For example, various basement membrane components, such as type IV collagen, laminin, fibronectin, and proteoglycans, in the human uterus undergo changes throughout the menstrual cycle and pregnancy . Likewise, the ECM components undergo remodeling during mouse uterine stromal cell decidualization . Matrix metalloproteinases and tissue inhibitors of MMPs are thought to be key mediators for matrix degradation during implantation and decidualization . There is evidence that a balance between a select set of MMPs and TIMPs is important for implantation. Mechanisms regulating the MMP and TIMP genes during the periimplantation period are not clear, although growth factors and cytokines including the EGF and TGF family members and LIF have been shown to modulate MMPs and TIMPs .
Recommended Reading: Age Word Problems Worksheet With Solutions
Contraception And Birth Control
The prevention of a pregnancy comes under the terms contraception or birth control. Strictly speaking, contraception refers to preventing the sperm and egg from joining. Both terms are, however, frequently used interchangeably.
| sterilization | less than 1% |
Table 24.3 lists common methods of contraception. The failure rates listed are not the ideal rates that could be realized, but the typical rates that occur. A failure rate is the number of pregnancies resulting from the methods use over a twelve-month period. Barrier methods, such as condoms, cervical caps, and diaphragms, block sperm from entering the uterus, preventing fertilization. Spermicides are chemicals that are placed in the vagina that kill sperm. Sponges, which are saturated with spermicides, are placed in the vagina at the cervical opening. Combinations of spermicidal chemicals and barrier methods achieve lower failure rates than do the methods when used separately.
Compliance with the contraceptive method is a strong contributor to the success or failure rate of any particular method. The only method that is completely effective at preventing conception is abstinence. The choice of contraceptive method depends on the goals of the woman or couple. Tubal ligation and vasectomy are considered permanent prevention, while other methods are reversible and provide short-term contraception.
E Signaling By Cytokines
LIF and its receptors, LIFR and gp130, exist in both soluble and membrane-bound forms, and soluble forms of these two receptors antagonize the actions of their ligands, implying the complexity of the LIF signaling pathway . Lif is transiently expressed in uterine glands on d 4 of pregnancy in mice, suggesting its role in implantation . However, our recent studies show that uterine Lif expression is biphasic on d 4. Not only is Lif expressed in glands, but it is also expressed in stromal cells surrounding the blastocyst at the time of the attachment reaction . This suggests that LIF has dual roles: first in the preparation of the uterus, and later in the attachment reaction. However, the molecular mechanism by which LIF executes its effects on implantation is not yet known. In this regard, it would be useful to establish the complicated ligand-receptor interactions and detailed expression patterns of LIF receptors that occur during the periimplantation period. However, a recent report shows that inactivation of gp130 by deleting all signal transducers and activators of transcription binding sites results in implantation failure , reinforcing the importance of LIF signaling in implantation.
Also Check: Abiotic Ecology Definition
A Steroid Hormone Signaling
A large variety of natural and synthetic compounds that mimic natural estrogens and bind to the nuclear ER are present in the environment . A few of these xenobiotics possess an even higher affinity for ER than for ER . The interaction of xenoestrogens with ER is considered as the basis for their reproductive toxicity, although their affinity for the receptor is quite low . However, there is evidence that responses to an estrogenic compound in target tissues are not necessarily related to its affinity for the receptor , suggesting the presence of other signaling pathways. Thus, xenoestrogens may interact with ER or other binding proteins that may not result in a similar kind of transactivation that normally occurs with natural ligands. Their estrogen-like effects in the uterus include an increase in water imbibition and ornithine decarboxylase activity, as well as increased DNA and protein synthesis. Xenoestrogens can also induce implantation in progesterone-primed rodents . Although the mechanisms of action of these xenoestrogens are not clear, these compounds have received a great deal of attention as a possible cause of certain cancers and impaired reproductive functions .
Reproduction Fertility And Contraception
Most animals carry out sexual reproduction. Sexual reproduction involves the joining of two sex cells the sperm and the egg/ovum .
nucleus and a haploid egg nucleus to form a diploid zygote.
A zygote is the first cell of a new individual. Fertilisation occurs in the oviduct.
- The zygote travels down the oviduct dividing by mitosis to form a ball of cells .
- When the embryo reaches the uterus, implantation occurs. This is when the embryo attaches to the thick uterus lining to receive nourishment.
- The embryo differentiates to produce a variety of tissues and organs.
- The embryo is referred to as a foetus when it begins to look more like a baby.
You May Like: What Type Of Math Do Architects Use
Symptoms Of Implant Placement
As there is no real correlation between the time of implantation and the occurrence of implantation symptoms, it is best to think about implantation symptoms and how they relate to early pregnancy rather than the time of implantation.
The following are the most common implantation symptoms of early pregnancy:
Implantation Cramps
Implantation cramps Some women may experience minor cramping right around the time of implantation, which is normal. Though there is no way to know for certain what is going on, we do know that this cramping is caused by a rise in progesterone that occurs during the second half of your cycle, regardless of whether or not you are pregnant.
Implantation Bleeding
Implantation bleeding Implantation bleeding is defined as a small amount of bleeding or spotting that can occur after conception and a few days before your menstrual cycle. Implantation bleeding is light in nature, stops on its own, and does not require medical intervention. It affects approximately one-third of all pregnant women, despite the fact that there is no scientific evidence to support a link between implantation and bleeding.
Nausea
Implantation symptoms in early pregnancy, and they are often some of the first indications that something is wrong with the baby. You may also begin to notice changes in your appetite or that you are suddenly disgusted by foods that you used to eat with gusto.
Constipation and Bloating
Fatigue.
1. What is Implantation in Biology?
V Window Of Implantation: A Transient And Unique Moment
In all eutherian mammals thus far studied, the uterus differentiates into an altered state when blastocysts are capable of effective two-way communication to initiate the process of implantation. This state is termed uterine receptivity for implantation and lasts for a limited period. At this stage, the uterine environment is able to support blastocyst growth, attachment, and the subsequent events of implantation . The major factors that specify uterine receptivity are the ovarian steroids, progesterone and/or estrogens. Ovarian progesterone and estrogen are crucial for implantation in mice and rats, but ovarian estrogen is not essential for implantation in pigs, guinea pigs, rabbits, and hamsters . Estrogen-synthesizing capacity has been demonstrated in rabbit and pig embryos, but whether embryonic estrogen plays a role in implantation in these species is still debatable. Recent evidence suggests that hamster blastocysts express the aromatase gene . The mouse embryo lacks aromatase activity necessary for estrogen synthesis . Whether preimplantation estrogen secretion by the ovary or embryo plays a role in human implantation is unknown.
Recommended Reading: Percent Difference In Physics